Patient Monitoring Equipment Explained: ECG, SpO₂, NIBP & More
Posted by Moshe M on 25th Feb 2026
A Complete Guide for Clinics, Hospitals, EMS & Long-Term Care in Canada
Introduction
In today’s healthcare environment, patient monitoring equipment is no longer limited to intensive care units. From small outpatient clinics to large hospitals, long-term care facilities, and EMS services, accurate and reliable monitoring devices are essential for delivering safe, high-quality patient care.
Understanding how monitoring equipment works — and when to use each type — helps healthcare providers make informed purchasing decisions and improve patient outcomes. This guide explains the core technologies behind ECG, SpO₂, NIBP, temperature monitoring, respiratory monitoring, and multi-parameter patient monitors, along with practical insights for Canadian healthcare facilities.
What Is Patient Monitoring Equipment?
Patient monitoring equipment refers to medical devices used to measure, display, and track a patient’s vital signs and physiological status. These devices provide real-time data that allows healthcare professionals to detect abnormalities early and respond quickly to changes in a patient’s condition.
Monitoring systems may be used continuously — such as in an ICU — or intermittently, such as during routine assessments in a clinic or long-term care facility. The goal is always the same: early detection, improved safety, and better clinical decision-making.
Common vital signs monitored include:
-
Heart rate and cardiac rhythm
-
Oxygen saturation (SpO₂)
-
Blood pressure (NIBP)
-
Respiratory rate
-
Body temperature
Modern healthcare increasingly relies on integrated monitoring systems that combine multiple parameters into one compact, easy-to-use device.
ECG Monitoring (Electrocardiography)
Electrocardiography, commonly known as ECG or EKG, measures the electrical activity of the heart. It is one of the most important diagnostic and monitoring tools in cardiovascular care.
How ECG Monitoring Works
The heart generates electrical impulses that cause it to contract and pump blood. ECG electrodes placed on the chest and limbs detect these electrical signals and translate them into waveforms displayed on a monitor or printed on paper.
These waveforms allow clinicians to assess:
-
Heart rhythm and rate
-
Conduction abnormalities
-
Signs of myocardial infarction (heart attack)
-
Electrolyte imbalances
-
Ischemia or cardiac strain
Types of ECG Systems
3-lead ECG monitoring is commonly used for basic rhythm monitoring in emergency rooms and inpatient wards.
5-lead ECG provides more detailed rhythm information and is often used in critical care settings.
12-lead ECG systems offer comprehensive diagnostic data and are widely used in cardiology, emergency departments, and pre-hospital EMS settings.
Why ECG Monitoring Is Essential
Continuous ECG monitoring allows healthcare teams to detect arrhythmias and cardiac instability before symptoms worsen. In emergency situations, rapid ECG interpretation can mean the difference between early intervention and delayed treatment.
Hospitals, ambulances, and cardiac clinics rely heavily on ECG monitoring to support cardiac patients and high-risk individuals.
SpO₂ Monitoring (Pulse Oximetry)
SpO₂ monitoring measures peripheral capillary oxygen saturation — the percentage of hemoglobin in the blood that is saturated with oxygen. It is a non-invasive and critical indicator of respiratory and circulatory function.
How Pulse Oximeters Work
A pulse oximeter uses light-emitting diodes (LEDs) to pass red and infrared light through a thin part of the body, typically a fingertip. A sensor detects how much light is absorbed by oxygenated and deoxygenated blood, calculating oxygen saturation levels and pulse rate.
Clinical Importance of SpO₂ Monitoring
Low oxygen saturation can indicate:
-
Respiratory distress
-
Pneumonia
-
COPD exacerbations
-
Pulmonary embolism
-
Anesthesia complications
-
Cardiac conditions
Pulse oximetry is widely used in emergency medicine, surgical suites, ICU settings, long-term care facilities, and even home healthcare.
Benefits of Modern Pulse Oximeters
-
Portable and lightweight designs
-
Quick, real-time readings
-
Battery-operated for mobile use
-
Integration with multi-parameter monitors
SpO₂ monitoring became especially critical during respiratory outbreaks and continues to be a standard in routine patient assessments.
NIBP Monitoring (Non-Invasive Blood Pressure)
Non-invasive blood pressure (NIBP) monitoring is one of the most commonly performed assessments in healthcare. Accurate blood pressure readings provide essential information about cardiovascular health and circulatory stability.
How NIBP Monitoring Works
An inflatable cuff is placed around the patient’s arm or leg. The device inflates the cuff to temporarily restrict blood flow and then gradually deflates it while measuring oscillations in arterial pressure. These oscillations are used to calculate systolic, diastolic, and mean arterial pressure.
Clinical Relevance of Blood Pressure Monitoring
Abnormal blood pressure readings may indicate:
-
Hypertension
-
Hypotension
-
Shock
-
Sepsis
-
Cardiac dysfunction
-
Medication effects
Routine NIBP monitoring is essential in nearly all healthcare environments, including clinics, hospitals, surgical units, and long-term care facilities.
Types of Blood Pressure Devices
-
Manual sphygmomanometers
-
Automated digital blood pressure monitors
-
Integrated NIBP modules within multi-parameter monitors
-
Ambulatory blood pressure monitoring systems
For high-risk or unstable patients, continuous or repeated automated monitoring is especially valuable.
Temperature Monitoring
Body temperature is a fundamental indicator of infection, inflammation, or systemic illness. Accurate temperature measurement supports diagnosis and guides treatment decisions.
Types of Medical Thermometers
Digital oral thermometers are commonly used in clinical and outpatient settings.
Tympanic thermometers measure temperature from the ear and provide rapid readings.
Infrared forehead thermometers allow contactless measurement and are widely used in triage settings.
Continuous temperature probes are used in critical care environments for ongoing monitoring.
Why Temperature Monitoring Matters
Elevated body temperature may indicate infection or inflammatory conditions, while low temperature can signal shock or metabolic disturbances. In pediatric and geriatric populations, careful monitoring of temperature changes is especially important.
Respiratory Rate Monitoring
Respiratory rate is one of the most sensitive indicators of patient deterioration. An abnormal respiratory rate often appears before other vital signs change significantly.
Importance of Respiratory Monitoring
An increased respiratory rate may indicate:
-
Respiratory distress
-
Sepsis
-
Metabolic acidosis
-
Anxiety or pain
A decreased respiratory rate may signal:
-
Sedation overdose
-
Neurological impairment
-
Respiratory failure
Respiratory monitoring may be performed manually or through integrated monitoring systems that track chest movement or impedance-based measurements.
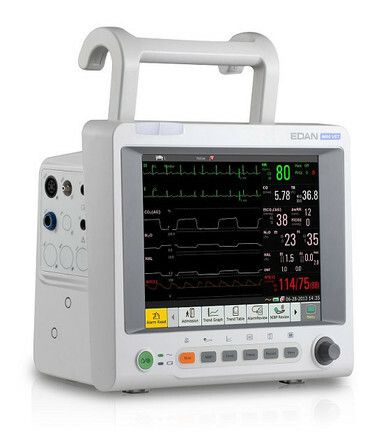
Multi-Parameter Patient Monitors
Multi-parameter monitors combine several vital sign measurements into one device. These systems are commonly used in hospitals, emergency departments, operating rooms, and critical care units.
What Multi-Parameter Monitors Measure
-
ECG (heart rate and rhythm)
-
SpO₂ (oxygen saturation)
-
NIBP (blood pressure)
-
Respiratory rate
-
Temperature
Some advanced monitors may also include invasive blood pressure, end-tidal CO₂ (capnography), and cardiac output monitoring.
Advantages of Integrated Monitoring Systems
Integrated monitors streamline workflow by consolidating data into a single display. They provide:
-
Real-time vital sign trends
-
Visual and audible alarms
-
Improved patient transport capabilities
-
Reduced equipment clutter
For EMS and transport teams, portable multi-parameter monitors ensure continuity of care from pre-hospital settings to emergency departments.
Choosing the Right Patient Monitoring Equipment
Selecting the appropriate monitoring equipment depends on several factors:
Clinical Setting
Intensive care units require advanced multi-parameter monitors with continuous waveform display and alarm capabilities. Outpatient clinics may only require automated blood pressure monitors and pulse oximeters.
Patient Population
Pediatric patients require appropriately sized cuffs and sensors. Geriatric patients may require more frequent monitoring due to comorbidities.
Portability
Ambulances and transport teams require compact, battery-powered devices. Long-term care facilities may prioritize ease of use and simplified displays.
Data Integration
Modern monitoring systems often integrate with electronic medical records (EMR) systems, allowing seamless documentation and centralized monitoring.
Why High-Quality Monitoring Equipment Matters
Reliable patient monitoring equipment improves patient outcomes by enabling early detection of deterioration. When vital signs are accurately measured and continuously tracked, clinicians can intervene before complications escalate.
Investing in professional-grade monitoring systems supports:
-
Reduced hospital readmissions
-
Improved cardiac and respiratory care
-
Enhanced patient safety
-
More efficient clinical workflows
-
Better compliance with healthcare standards
Accurate monitoring devices also reduce the risk of false readings and unnecessary interventions.
The Future of Patient Monitoring in Canada
Healthcare in Canada continues to evolve toward more connected and data-driven systems. Emerging trends in patient monitoring include:
-
Wireless and remote patient monitoring
-
AI-assisted early warning systems
-
Telehealth integration
-
Compact wearable monitoring devices
-
Improved infection control designs
As technology advances, monitoring systems will become even more precise, portable, and integrated with broader healthcare networks.
Final Thoughts
Patient monitoring equipment — including ECG systems, pulse oximeters, non-invasive blood pressure monitors, and multi-parameter devices — forms the backbone of safe, modern healthcare delivery.
Whether in hospitals, clinics, EMS units, or long-term care facilities, accurate monitoring supports early detection, informed decision-making, and improved patient outcomes.
Understanding how each device works and selecting the right equipment for your facility ensures that healthcare professionals are equipped to provide safe, efficient, and high-quality care across all clinical settings.